We Can Reach the Finish Line on Health Coverage for Hispanic Kids
By Sonya Schwartz, Research Fellow, Center for Children and Families, Georgetown Univeristy
(cross-posted from “Say Ahhh!” children’s health policy blog)
 Ensuring that every child in America has the protection of health care coverage is an attainable goal. In partnership with National Council of La Raza, this week we released a 50-state analysis of health coverage for Hispanic children. Our analysis found that Washington, DC is just a step away from the finish line already with 99 percent of Hispanic children covered, and other states have also made enormous strides.
Ensuring that every child in America has the protection of health care coverage is an attainable goal. In partnership with National Council of La Raza, this week we released a 50-state analysis of health coverage for Hispanic children. Our analysis found that Washington, DC is just a step away from the finish line already with 99 percent of Hispanic children covered, and other states have also made enormous strides.
The U.S. as a whole is also making steady progress, with the number of uninsured Hispanic children dropping by more than half a million from 2009 to 2013. However, despite this progress, two million Hispanic children continue to be uninsured, and Hispanic children are one and a half times more likely to be uninsured than all children.
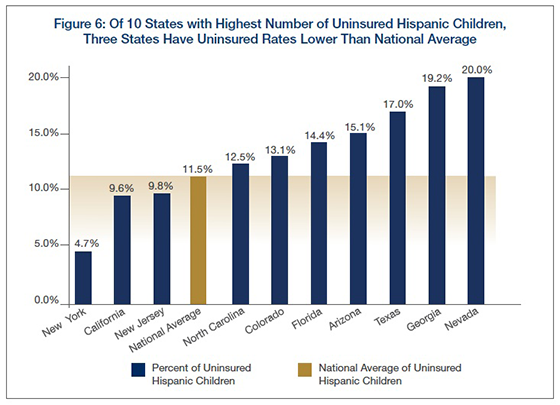
Which States Are In the Lead? About 80 percent of uninsured Hispanic children live in ten states—Texas, Florida, Arizona, Georgia, Nevada, Colorado, North Carolina, California, New York, and New Jersey. Three of these states —New York, California, and New Jersey—have brought their uninsured rate for Hispanic children below the national average.
What is the Special Sauce that Helps these States Succeed? There are a few ingredients that successful states have in common, and they all have to do with addressing barriers to coverage. Some of the key barriers include:
- Fear: The vast majority (93 percent) of Hispanic children are citizens, but some live in families where their parents are not. Communicating to parents that it is safe to apply for health coverage for their children regardless of their own immigration status, and supporting trusted sources in encouraging them to do so, is a must.
- Language: Limited English proficiency is a major barrier to coverage for parents trying to enroll their children in coverage and keep them enrolled. About one third (32.3 percent) of the U.S. Hispanic population over the age of five has limited English proficiency. With three fourths (73.3 percent) of this population speaking Spanish, it is important to create culturally appropriate health insurance outreach materials in Spanish in order to enroll eligible but uninsured children.
- Paperwork: Getting through the application or renewal process for coverage can be daunting for all families, and is particularly hard for families applying for the first time or families that do not speak English well. The Affordable Care Act provided additional resources for enrollment assistance to more than 10 million people, yet not nearly enough resources to reach the bulk of the uninsured. Continuing to provide resources at all levels for enrollment assistance programs in trusted community environments makes a world of difference.
- Coverage for parents as well as kids: Many of the the states that were most successful in improving Hispanic kids coverage not only provide affordable coverage for children, but also have had a commitment to providing affordable coverage for their parents. Research has shown that covering parents reduces the number of uninsured children.
Health coverage isn’t just about getting health care when you need it, it’s linked to school success, and improved financial security for families so we need to keep working to close this coverage gap. Strong Medicaid and CHIP programs have helped improve health coverage for a generation of America’s children.
This open enrollment period is a great opportunity to reach Hispanic families and encourage them to enroll for coverage along with their children. And we can encourage families to enroll their kids in Medicaid and CHIP all year long. Let’s build on this momentum and get all kids the coverage they need to succeed.